First Aid Procedure for Thermal Burns
Thermal burns are one of the most common types of injuries encountered in daily life, work, and industrial accidents. The treatment of thermal burns must adhere to a standardized procedure, based on the pathophysiology of heat-induced injury and fundamental first aid principles. Proper first aid for thermal burns not only provides immediate pain relief but also helps limit the spread of tissue necrosis, prevent infection, and reduce scarring and other sequelae.
1. Overview of Thermal Burns
1.1. Mechanism of Skin Injury Caused by Thermal Burns
There are many types of burns, such as thermal burns, chemical burns, electrical burns, etc. Among them, thermal burns are the most common type, primarily occurring in daily life. Thermal burns are categorized into dry heat and wet heat (scalds). Dry heat burns result from contact with a hot iron, a hot motorcycle exhaust pipe, fires, gas explosions, etc. Wet heat burns originate from contact with boiling water, hot soup, hot steam, etc. When the skin and underlying tissues are exposed to heat that exceeds their physiological tolerance, the cellular structure is destroyed, causing thermal burn injuries that range from superficial to deep, and localized to widespread.
Specifically, when heat acts on the skin, the thermal energy denatures proteins and disrupts cell membranes and local microvessels. In mild cases, the injury is localized to the epidermis, causing redness and a burning sensation. In severe cases, the heat penetrates deep into the dermis, subcutaneous tissue, and even reaches the muscles and bones, causing blistering, necrosis, and circulatory disorders in the burned area. A thermal burn injury doesn't just stop at the initial point of contact; it tends to spread during the first few hours due to inflammatory responses and microcirculatory disorders. Therefore, early and proper first aid intervention helps interrupt the tissue destruction process, reducing the area and depth of the injury.

First aid for thermal burns must be administered right at the scene, before bandaging or taking the victim to a medical facility.
1.2. Classification of Thermal Burn Severity
Thermal burns are typically classified by the depth of the injury. Recognizing the severity of a thermal burn during first aid helps determine the appropriate response, assess the need for hospital transfer, and monitor the condition. Thermal burns consist of 3 main degrees:
-
First-degree burns: Affect only the outer layer of the skin (epidermis). Symptoms include red, painful skin that turns white when touched, with no blistering or pus.
-
Second-degree burns: Cause damage to the epidermis and part of the dermis (the second layer of skin). Mild manifestations include red, painful skin that turns white upon touch, blistering, and intact hair follicles. Severe manifestations may or may not be painful (the wound might be so deep that nerve endings are severed), can be wet or dry (deep enough to destroy sweat glands), may turn white when touched, and body hair in the area falls out.
-
Third-degree burns: The most severe type. The burn wound involves both the epidermis and the dermis. Nerves, blood vessels, and hair follicles are completely destroyed. If the burn is extremely severe, it can affect underlying bones and muscles.
Clinical studies show that the first 10 to 30 minutes after a thermal burn is a critical window to reduce the residual heat trapped in the tissues. If not cooled down promptly, the necrotic process continues, making the burn deeper and more widespread. Thus, first aid must be initiated immediately at the scene.
2. Proper First Aid Procedure for Thermal Burns
Step 1: Remove the causative agent and get the victim out of the danger zone
The first and most crucial rule in any emergency is to cut off the source of harm. Upon discovering the incident, quickly remove the victim from the fire, boiling water, or hot objects. If the victim's clothes are on fire, instruct them to stop, drop, and roll on the ground to extinguish the flames; they must absolutely not run, as the wind will fan the flames. Once safe, quickly remove clothing, shoes, or jewelry from the burned area before the wound begins to swell. However, a critically important note in this step: if the clothing has burned and melted into the wound, absolutely do not forcefully peel it off. Doing so will rip off the skin, cause excruciating pain, and increase the risk of infection. In this case, only use scissors to cut away the surrounding clothing and leave the stuck portion for medical professionals to handle later.
Step 2: Soak, wash, and cool the injured area
This is the most important step determining the wound's recovery level. Immediately after separating from the heat source, the burned area must be cooled with clean water.
-
Type of water: Clean, cool water is best, at a temperature of about 16 to 20°C. You can use boiled water that has cooled down, or clean lake/river water if far from residential areas. Absolutely do not use ice or apply ice directly.
-
Method: Directly soak the burned area in a basin of cool water or gently run it under a tap. Running water must be applied carefully; avoid high water pressure that could cause pain or rupture blisters.
-
Duration: Maintain cooling for 15 to 30 minutes, or until the victim feels less burning pain.
-
Effect: Timely cooling lowers the skin's surface temperature, stopping heat from penetrating deeper into underlying tissues, thereby minimizing the burn's depth. Additionally, cool water effectively reduces pain and swelling.
-
Note: For children or during winter, when applying this step, ensure you only cool the burned area while keeping the rest of the body warm. Do not submerge a child's entire body in cold water for too long to prevent sudden hypothermia, which can cause arrhythmias or cardiac arrest.
Step 3: Cover and protect the wound
After cooling, the greatest risk to a thermal burn is bacterial invasion from the external environment. Since the protective skin layer is damaged, bacteria can easily attack, potentially causing sepsis. To safely handle the burn at this stage, use sterile medical gauze or a clean cloth to gently cover the wound. Bandage loosely; do not wrap too tightly to ensure proper blood circulation and avoid compressing the swelling tissue.
-
Note: Absolutely do not use cotton balls to cover a burn. The small cotton fibers easily stick to the wound's exudate and form a hard crust when dry, causing immense pain and difficulty for doctors when changing bandages later. If the burn is on an arm or leg, keep the injured limb elevated to reduce swelling caused by blood pooling.
Step 4: Rehydrate, replenish electrolytes, and prevent shock
Large-area thermal burns often cause the body to lose a massive amount of water and blood plasma through the wound, leading to hypovolemic shock. Therefore, fluid resuscitation is extremely necessary. If the victim is conscious and has no abdominal injuries, give them fluids to replace what was lost. Recommended drinks include: Oresol solution, warm sweet tea, thin rice gruel, mineral water, or fruit juice. Avoid giving large amounts of plain water alone, as it can cause electrolyte imbalances. Simultaneously, lay the victim in a comfortable position, with the head low or flat to allow easy blood flow to the brain. Keep the victim warm with a light blanket and reassure them to reduce panic and pain. For extreme pain, common over-the-counter painkillers can be used, but with caution and ideally under medical advice.
Step 5: Transfer the victim to a medical facility
Not all thermal burns can be treated at home. Quickly transfer the victim to the nearest medical facility if you observe the following signs:
-
Large area burns or deep burns (2nd or 3rd degree).
-
Burns located in critical areas such as the face, neck, airway (due to inhaling hot smoke), hands, feet, or genitals.
-
The victim is a child, an elderly person, or someone with an underlying medical condition.
-
Signs of heat shock: rapid pulse, low blood pressure, profuse sweating, drowsiness, etc. During transport, ensure the victim is kept warm and closely monitor their breathing and circulation. If the victim stops breathing or their heart stops, perform Cardiopulmonary Resuscitation (CPR) immediately.
3. Mistakes to Avoid During Thermal Burn First Aid
Despite widespread education on proper burn first aid, many dangerous misconceptions persist, hindering treatment. In reality, many cases of thermal burns worsen due to improper first aid. Here are typical mistakes:
-
Applying ice directly: Many people believe ice cools the burn faster. However, this is an extremely dangerous action. The burned skin is very fragile; sudden exposure to freezing temperatures causes blood vessels to constrict, reducing blood supply to the injured area and making the burn deeper. This action can even cause "frostbite" on top of the thermal burn, leading to rapid tissue necrosis.
-
Applying foreign substances to the burn: Folk remedies often suggest applying toothpaste, python fat, fish sauce, egg whites, or various leaves to soothe a burn. In reality, these substances not only fail to cool or heal the wound, but they also act as an ideal breeding ground for bacteria, causing severe infections. Furthermore, upon arriving at the hospital, doctors will have to spend a lot of time scraping and cleaning these substances off, causing the victim agonizing pain.
-
Popping blisters: Blisters are actually a highly valuable natural biological dressing that helps protect the delicate new skin underneath from bacteria and dehydration. Intentionally popping or tearing these blisters equates to opening a direct doorway for bacteria to invade the inner tissues. Let the blisters deflate or break naturally during the healing process.
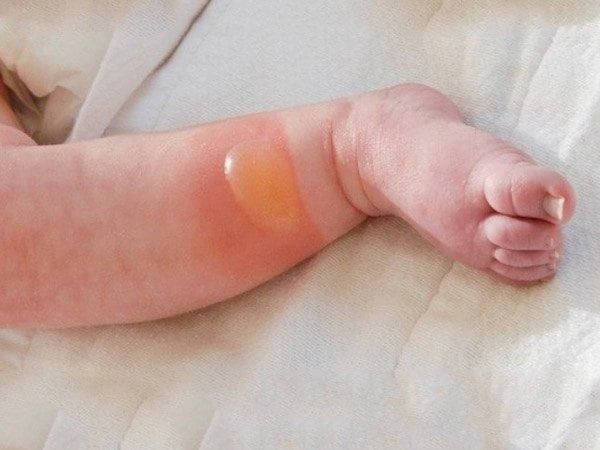
Blisters play a role in protecting the underlying skin from bacteria during the healing process.
4. First Aid for Thermal Burns in Special Groups
The basic first aid procedure is theoretically the same, but applying it to specific demographics requires flexibility and more specialized knowledge. Particularly for children and the elderly, minor errors in first aid can lead to life-threatening complications much faster than in healthy adults.
4.1. Children
A child's skin structure is not fully developed; their epidermis is much thinner than an adult's. Therefore, with the same temperature and exposure time, an adult might only suffer skin redness (1st degree), while a child could suffer deep 2nd or 3rd-degree burns. The ratio of skin surface area to body weight in children is also larger, meaning dehydration and hypothermia occur extremely rapidly. Intervention should focus on the following:
-
Body temperature control: After cooling the wound, remember to only cool the burned area; do not submerge the child's entire body in cold water. Parents must immediately keep the rest of the child's body warm with a dry blanket or clean towel. Letting a child shiver from the cold will worsen shock, cause arrhythmias, and lead to respiratory failure.
-
Psychological and airway stabilization: Burned children usually panic, scream, and cry violently. This not only makes first aid difficult but also increases pressure on the respiratory system, easily leading to laryngeal spasms or choking. Comforting, holding, and reassuring the child at this moment is just as important as medical intervention.
-
Careful rehydration: When giving a child electrolyte fluids, do it slowly, in small spoonfuls. Avoid forcing the child to drink too fast, which can cause vomiting and the life-threatening risk of aspirating vomit into the lungs.
4.2. Elderly and People with Underlying Conditions
For the elderly and individuals with underlying conditions like cardiovascular disease or diabetes, the risk of infectious complications and delayed wound healing is much higher. Thus, first aid must be performed carefully, monitored closely, and followed by early hospital transfer. Intervention should focus on:
-
Reduced sensation and reflexes: The elderly, especially diabetics with peripheral neuropathy, often have reduced sensitivity to pain and heat. This causes them to notice the accident late, leading to prolonged contact with the heat source and allowing the burn to penetrate deep into tendons and muscles without their awareness.
-
Weakened immune system: The resistance of this group is very poor, combined with an aging circulatory system that nourishes the skin, making burns very hard to heal and increasing the infection risk exponentially. A small burn, if not properly treated with first aid and kept sterile, can quickly progress to necrosis and sepsis.
-
Cardiovascular complications: The intense pain and panic from a burn can trigger heart attacks, sudden blood pressure spikes, or strokes right at the moment of the accident. Therefore, first aid must be very gentle to avoid causing severe agitation. Monitor their heart rate and breathing closely, and move them to a medical facility early, regardless of the burn's size.
Thermal burn accidents can leave lifelong sequelae. Mastering standard, medically accurate first aid procedures is essential knowledge for everyone. Calmness and precise actions in the first few minutes are the best medicine to minimize burn damage, prevent infection, and support the future healing process. Eliminate incorrect first aid habits immediately and proactively participate in skills training courses so you can confidently protect yourself and those around you from life's risks.
References:
-
Nguyen Tri Phuong Hospital, First aid and emergency procedure for thermal burn injuries, accessed at: https://bvnguyentriphuong.com.vn/chan-thuong-chinh-hinh/quy-trinh-so-cuu-cap-cuu-ton-thuong-bong-nhiet
-
Vinmec International General Hospital, Correct first aid when suffering from exhaust pipe burns, thermal burns, accessed at: https://www.vinmec.com/vie/bai-viet/so-cuu-dung-khi-bi-bong-bo-bong-nhiet-vi
Comments:
There are no comment for this news.
 Tiếng anh
Tiếng anh  Vietnam
Vietnam 






.png)
.png)

